Y’all. It’s only been 4 days so far since I turned on the Control IQ feature -but I am LOVING it and can’t believe I’ve gone almost 28 years with diabetes and didn’t have this technology. It is amazing. When I was explaining to my 12 year old what it is he even asked me, “Why hasn’t that always been a thing?”
I have been in range the entire time, with the exception of a few blips here and there. The first night I dropped to around 70 at 3am and I got the alarm but it suspended my pump and I came right back up. I stayed awake for a bit just to see if I needed to treat it but I was good and woke up in the 120s.
A couple of times I have popped up a little over 200 but those times have all been food related and from bad food swags. #ithappens But the pump quickly corrected and brought me back down into range.
I have found that I am also taking less insulin as a whole during the day. I assume it is because “before” I might not correct soon enough and therefore my bg would be higher and would require more insulin. Now that the pump is catching the highs sooner, it requires less of a correction, therefore I am using less total insulin.
Also I have done a workout every day using the exercise feature and that has worked like a charm every time, too. I no longer spike up way over 200 then drop down an hour or so later. I’ve stayed in the 120-140 range during the workout and stay steady afterward.
I feel like I should hear angels singing or something ….
I have been stalking friends who have been using this technology and I kept thinking “Ok great it works for them but not sure how it would work for ME.” But let me tell you .. I am 100% happy I made the switch and have been VERY impressed with it so far.
Last night I met some friends for Happy Hour and I was tempted to see what it would do with a sweet drink – which I love but usually try to avoid because I don’t want to deal with the high bg’s afterwards. But I chickened out and went the safe route and had a Diet Coke and vanilla rum. No blip at all in my graph – boom. Next time I’ll try to be more adventurous, though. ;). Everyone is different but what I have found in the past is the juice will raise it but sometimes the liquor will drop it so it evens out -but I try to not do a straight up juice mixed drink because that’s gonna just make me skyrocket. #YDMV But if I do get brave, I’ll let ya know.
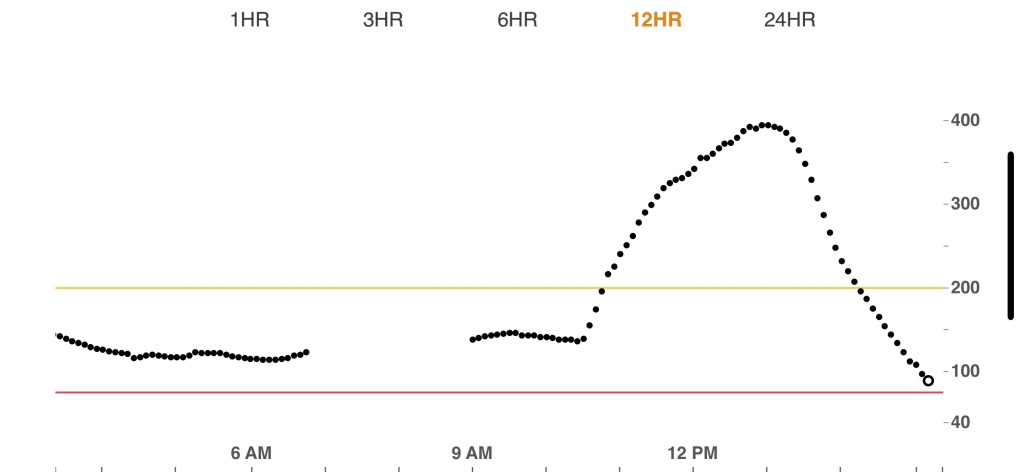
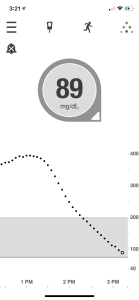
Below is my Dexcom graph for the last 24 hours. For those that aren’t familiar, the gray area is my ideal range. You can see that yesterday evening a little before 6pm I got up a little bit out of range, but then came back down (I think I had a snack I didn’t bolus for). It is perfectly normal to have some peaks and valleys within the range – nobody’s blood sugar stays 100% straight all the time – because aaaalll the things affect blood sugar. But as long as I’m staying in that gray range, I am golden. 🙂



 I have been going to our local JDRF walk since 1993 – it doesn’t feel that long but sheesh this year will be what, 28 years? Whoa. I need to let that soak in for a minute. I’ve only missed a handful of years; the first two times I missed it was because I was in DKA, so I suppose that’s a valid reason, right?
I have been going to our local JDRF walk since 1993 – it doesn’t feel that long but sheesh this year will be what, 28 years? Whoa. I need to let that soak in for a minute. I’ve only missed a handful of years; the first two times I missed it was because I was in DKA, so I suppose that’s a valid reason, right?